Diabetic Foot
Diabetic foot disease is any condition that results directly from peripheral artery disease (PAD) or sensory neuropathy (DPSN) affecting the feet of people living with diabetes. Diabetic foot conditions can be acute or chronic complications of diabetes. Presence of several characteristic diabetic foot pathologies such as infection, diabetic foot ulcer and neuropathic osteoarthropathy is called diabetic foot syndrome. The resulting bone deformity is known as Charcot foot.
Due to advanced peripheral nerve dysfunction associated with diabetes (diabetic neuropathy), patients' feet have a dryness of the skin and a reduced ability to feel pain (nociception). Hence, minor injuries may remain undiscovered and subsequently progress to a full-thickness diabetic foot ulcer.
Research estimates that the lifetime incidence of foot ulcers within the diabetic community is around 15% and may become as high as 25%.Where wounds take a long time to heal, infection may set in, spreading to bones and joints, and lower limb amputation may be necessary.
Foot infection is the most common cause of major leg amputation in the country (60-70%).
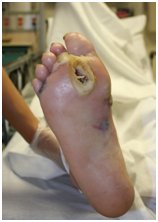
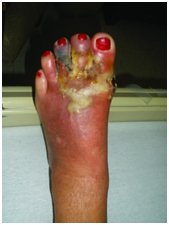
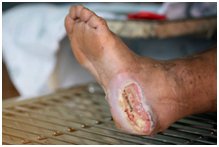
Diabetes Foot Care Guidelines
Diabetic foot care is essential as diabetes can be dangerous to your feet—even a small cut can produce serious consequences. Diabetes may cause nerve damage that takes away the feeling in your feet. Diabetes may also reduce blood flow to the feet, making it harder to heal an injury or resist infection. Because of these problems, you may not notice a foreign object in your shoe. As a result, you could develop a blister or a sore. This could lead to an infection or a nonhealing wound that could put you at risk for an amputation.
To avoid serious foot problems that could result in losing a toe, foot or leg, follow these guidelines.
Inspect your feet daily. Check for cuts, blisters, redness, swelling or nail problems. Use a magnifying hand mirror to look at the bottom of your feet.
Bathe feet in lukewarm, never hot, water.
Be gentle when bathing your feet.
Moisturize your feet but not between your toes.
Cut nails carefully.
Never treat corns or calluses yourself.
Wear clean, dry socks.
Keep your feet warm and dry.
Never walk barefoot. Not even at home! Always wear shoes or slippers.
Keep your blood sugar levels under control.
Do not smoke
Get periodic foot exams.
Treating Diabetic Foot Ulcers
- Medications: Antibiotics, antiplatelets, antipressure treatments.
- Off-loading: Stay off your feet to prevent pain from ulcers. It’s helpful for all forms of diabetic foot ulcers. Pressure from walking can make an infection worse and an ulcer expand, or to prevent recurrence.
- Shoes designed for people with diabetes, casts, foot braces, compression wraps, shoe inserts to prevent corns and calluses.
- Surgically remove foot ulcers with a debridement, the removal of dead skin or foreign objects that may have caused the ulcer.
- An infection is a serious complication of a foot ulcer and requires immediate treatment. Not all infections are treated the same way.
- Tissue surrounding the ulcer may be sent to a lab to determine which antibiotic will help. X-ray / MRI to look for signs of bone infection.
- Vaccuum Assisted Therapy (Negative pressure wound therapy – NPWT) is also offered for some deep seated wounds.
- Removing foot abnormalities such as bunions or hammertoes.
- Keller’s Arthroplasty, open flexor tenotomy, Weil’s Osteotomy, Jones EHL Tenosuspension, Tendon transfer, Gastrocnemius recession, TA lengthening, FHL Transfer to TA.

